- News and Stories
- Blog post
- Principles & Practices
Identifying Use Cases for AI in Medicaid Delivery

Identifying the right use cases for AI in Medicaid isn’t about chasing shiny technology—it’s about grounding innovation in the lived experiences of the people who rely on the program every day. At Code for America, we’ve seen how thoughtful, human-centered design can transform public systems, and AI is no exception. When applied responsibly, AI can help surface insights, reduce administrative burdens, and free up human capacity for what matters most: serving people with dignity and efficiency.
The key is starting with real problems, shaped by real stories from caseworkers and clients. The opportunity is significant—if we begin with the right questions.
When to use AI—and when not to
As part of our Government AI Landscape Assessment, we analyzed what types of use cases exist for AI in government. We came up with the following general rules for when generative AI is and isn’t the right tool for the job.
When is generative AI the right tool for the job?
- You have unstructured data you need to present in a structured way
- You need high-level analysis of a large amount of unstructured information
- You need to make policy, notices, or other documents easier for people to understand
- You need a solution for a labor intensive task involving unstructured data
- You have plans and resources to monitor performance over time
When is generative AI not the right tool for the job?
- You need precise outputs from structured information
- You need to do math with repeatable and reliable calculations
- You are unable to monitor performance over time
- You need human judgment to make a critical decision
Medicaid systems present a good testing ground for AI solutions
To start, let’s think of Medicaid systems as businesses with online sales. But within these systems, the sales inventory is not connected to the point of sale or client-facing website, the customer relations management system is outdated and takes nine months to make any changes, and critical documents are stored in a warehouse a block away.
Fixing all these problems manually would take an incredible amount of labor and time. But with creative uses of AI, we can start to approach solutions. With all of our solutions, we keep in mind that eligibility workers are the frontlines of state Medicaid programs, so anything we design has to meet their needs.
Using problem statements to identify solutions
In the human-centered design process, we start by looking at problem statements. We create these problem statements based on our user research with caseworkers, and find that they’re representative of the patterns that we see in our qualitative data. Let’s take a look at three different sets of problem statements, and the potential AI solutions we could apply to solving them.
I waste time navigating confusing menus and unnecessary screens.
I am forced to manually re-enter the same client data, which is slow and causes errors.
These problem statements, coming from the perspective of eligibility workers, lead us to two AI opportunities, both related to pulling info from documents.
First, we can use AI to pre-populate case management software to address the manual data entry issues. Second, we know that data also exists in many different documents in the benefits application and renewal process—so we ask, are there ways to pull data from these various documents and then use that data for verification?
The challenge—and the reason AI makes for a good solution—is that documents contain unstructured data, which can’t be easily read by computers. To make it more readable by machines, we can use AI to retrieve the data from a document, like names and dates and addresses, and label those pieces of information with some attribute.
At Code for America, we’ve applied this technique to look at court records and find information like court type, county, and other types of information that we could put into a database or another format for a computer to be able to read with more structure, enabling automated record sealing.
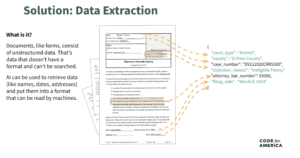
In this case, a state could create a tool that combines traditional machine learning and AI functionality to pull relevant information from back-end data matches and user-submitted documents to pre-populate screens in the worker’s eligibility system. The tool could provide easy access to the source documents so that workers can check for accuracy.
I find it difficult to make confident decisions because of inconsistent screens and information overload.
This problem statement opens another opportunity for AI to be applied. This time, let’s use AI to create a single trusted profile for every applicant, construct a complete view of the members of a household, and link applicants across benefits programs (like SNAP and Medicaid). Government often works with duplicative and messy legacy data, where multiple records for the same person exist across multiple systems. A process called entity resolution can help identify and link those records.
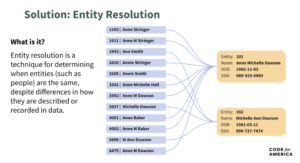
In this case, a state could use an AI-enabled entity resolution tool to flag relevant data across state systems, so that workers don’t miss key documentation, and can have a complete picture of eligibility.
I have to interrupt my work to look up policy rules in a separate system.
I spend too much time on case documentation instead of helping clients.
These problem statements illustrate a common problem for caseworkers. Here, we can use AI in a few different ways—we could create at-a-glance summaries of case notes and case narratives, summarize relevant policy in easy-to-read training guides for caseworkers, and create notices in plain language to provide clear information to enrollees (thereby taking some of the load off caseworkers).
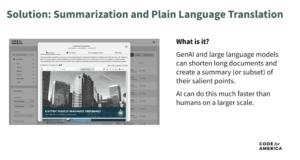
In this case, a state could use LLM to build functionality into existing case management systems. This LLM could provide a case summary based on all of the notes made on the case, create an internal chatbot to summarize policy for staff, and make plain language notices to explain case decisions to clients. We worked on a similar solution for governments that can parse through PDFs and create summaries to make them easier to sort—so we know that it can be done!
AI can make it easier to deliver Medicaid
The promise of AI in Medicaid will hinge on our collective commitment to designing with, not for, the people who use case management systems each and every day. By testing responsibly and measuring our progress along the way, we can ensure AI strengthens the systems people depend on. This moment is an invitation to build smarter, more responsive public services, grounded in compassion and evidence. If we remain focused on human outcomes, AI can help Medicaid deliver on its purpose: making care accessible, reliable, and simpler for everyone who needs it.